
Business Talk—In living colour: Why virtual visits cannot replace musculoskeletal care
Anthony Lombardi
Features Clinical Patient Care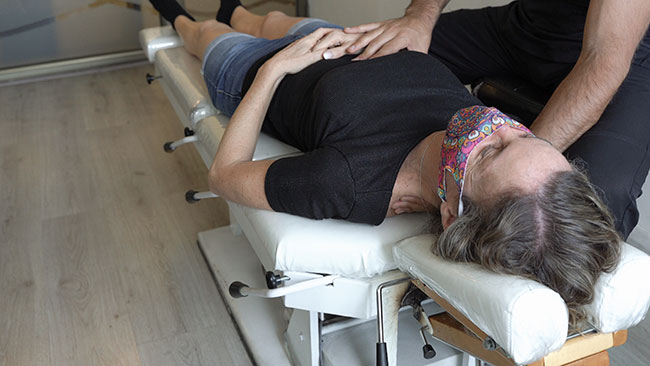 Photo: © Josu Ozkaritz / Adobe Stock
Photo: © Josu Ozkaritz / Adobe Stock A patient has on-going low back pain for the last five months. The pain progressively gets worse, while also travelling around the front of her torso. Although reluctant to see a health professional due to COVID-19, the patient finally makes an appointment with her primary care physician. Due to the same pandemic fears, he is only doing traditional phone-call appointments. During the call, the patient describes the pain, the location, and the history, and the doctor prescribes an anti-inflammatory and a muscle relaxant. Two weeks pass and she has no change in her pain. She calls her neighbour, a chiropractor, with whom she played soccer with in a women’s league. During the initial in-person visit, the chiropractor has the patient seated on the table and instantly notices what might be rib-humping coming from her back. She asks her patient to kindly remove her shirt so she can do an assessment. Instantly the chiropractor notices a mass protruding from the patient’s back. She asks the patient about it to get a history on her observation, but the patient knows nothing about this discovery. The patient is referred to a walk-in clinic where the medical doctor on call arranges a diagnostic ultrasound and plain film radiographs. Results indicates that the patient has an aggressive tumour which has eroded parts of the ribs and vertebrae.
This is happening today. Phone call or video doctor appointments run the risk of misdiagnosing or even worse – being unable to do a proper musculoskeletal assessment. Video conferencing is a little more descriptive to the physician versus the telephone, but both limit the ability of the doctor to use their clinical skills.
Telemedicine in the musculoskeletal arena should only be an adjunctive service. Relying totally on remote video or telephone patient visits is essentially leaving the physician in the dark. Many times, the patient has researched their symptoms on the Internet and the doctor tries to put the clues together. Usually, the doctor is led into the direction the patient has led them.
What is telemedicine?
Using remote technology like the traditional telephone or smartphone applications, the patient essentially describes their symptoms to the doctor, who then recommends treatment options. However, there are dangers of providing medical care for a musculoskeletal complaint from a such a distance. The main reason? Doctors of all kinds can’t properly assess their patients.
Wayne J. Guglielmo, MA, wrote a published report in September 2020 for the malpractice insurance company, The Doctors Company, summarizing the risks of telemedicine. The risks included: the possibility of suboptimal diagnoses and treatments, along with the added threat of failure to refer.
In another research study that was published in the Journal of the American Medical Association, Resneck et al reached similar conclusions. After analyzing the results of 62 clinical encounters from 16 different clinicians, they found that major diagnoses were repeatedly missed, and sometimes the patients were prescribed treatments that were not conguent with existing guidelines. The study concluded that while telemedicine has the potential to expand access to high-value healthcare, the findings of the research raise concerns about the quality of diagnosis and treatment options offered by telemedicine.
Malpractice
Legally, doctors must adhere to the standard of care that is same as treating them in person. In an interview with canadianlawermag.com, Darryl Cruz, a medical malpractice defence lawyer in Toronto says that the standard of care involves judging whether a doctor’s treatment for a patient or actions are reasonable and comparable to what another doctor would do in the same circumstance. In the same article, Duncan Embury, another medical malpractice lawyer, says the threshold for passing a virtual patient on and getting them into the hands of some other professional for in-person diagnosis may well be lower which could expose doctors’ liability.
The numbers
Ten percent of all primary care physician visits are due to musculoskeletal complaints. After cardiovascular disease, insurance companies spend the most money on visits, therapies, medicines, and surgeries related to muscle and joint pain. In my opinion, musculoskeletal patients need to be COVID-screened by primary care physician offices on the phone, and in-person appointments must be standard practice. Both doctor and patient need to take the appropriate precautions (wearing masks, and sanitizing regularly), but these patients need to be seen in-person to ensure they receive the best care possible. After all, chiropractors have been seeing patients in person for over a year, right from the beginning of the pandemic. We have donned masks and assessed and treated regardless. I feel that patients and physicians may be developing a false sense of security by thinking remote visits are stand-alone for musculoskeletal care.
At best, remote technology visits should be a screening tool for musculoskeletal conditions until an in-person visit can be arranged. Conversely, patients have other options. If they feel comfortable they can always visit their chiropractor in-person to be assessed or they can visit a primary care doctor at the many in-person walk-in medical clinics.
Anthony LOMBARDI, DC, is a private consultant to athletes in the NFL, CFL and NHL, and founder of the Hamilton Back Clinic, a multidisciplinary clinic. He teaches his fundamental EXSTORE Assessment System and practice building workshops to various health professionals. For more information, visit www.exstore.ca.
This article was originally published in the May-June 2021 edition of Chiropractic + Naturopathic Doctor. The original published title read “Why in-person visits cannot replace musculoskeletal care” and should have read as above (Why virtual visits cannot replace MSK care.) We regret the error.
Print this page