
Understanding motor muscle inhibition in musculoskeletal injury
Anthony Lombardi
Features Clinical Techniques acupuncture chiropractic electroacupuncture injury Motor point stimulation msk muscle inhibition musculoskeletal musculoskeletal assessment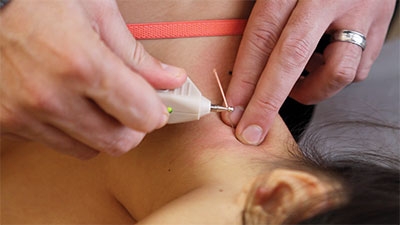 Photos courtesy of Hamilton Back Clinic
Photos courtesy of Hamilton Back ClinicUnderstanding the role of motor muscle inhibition in musculoskeletal injury, along with mastering the knowledge of accessing motor points, can revolutionize your practice.
Understanding the role of motor muscle inhibition in musculoskeletal injury, along with mastering the knowledge of accessing motor points, can revolutionize your practice. Making motor points a part of your regular treatment regime can help correct dysfunction and reduce motor inhibition, which can provide lasting clinical results.
How does motor muscle inhibition happen?
Motor muscle inhibition (alpha-motor neuron muscle inhibition) happens when the nerve that sends the impulse to contract the muscle becomes unable to function at its optimal capacity due to chemical or physical trauma. Direct or repetitive trauma and changes in the joint like inflammation, swelling or arthritis will trigger changes in the Golgi tendon organs (GTO) of the muscle. So, any trauma, pain, nociception or neurogenic inflammation in the region of the joint or muscle belly can trigger a modification of afferent information within the muscle spindles – causing motor inhibition.
Motor point stimulation
Whether done manually, with an acupuncture needle, or intramuscularly, motor point stimulation in the belly of a muscle stimulates the extrafusal fibre portion of the muscle spindle, which indirectly regulates the intrafusal fibre portion of that muscle restoring activation and muscle length within that motor unit. This restores biomechanical function in injured tissues along the kinetic chain of movement, modifies perfusion to trophic tissue and regulates proprioceptive function within that neuromuscular-articular region.
What treatments are used to stimulate motor points and restore motor inhibition?
There is a common misconception that a needle technique such as acupuncture or intramuscular stimulation must be used to restore motor function. Acupuncture, electroacupuncture and intramuscular stimulation are all effective in the activation of the motor point in an inhibited muscle. However, manual muscle release, deep tissue massage and trigger point therapy will also restore motor function if applied directly to the motor point itself.
Where are motor points located?
Motor points are found in the belly of all skeletal muscles. However, research has demonstrated that there is no consistent way of locating them in clinical practice. Some muscles like the pronator teres and anconeous have only one clinically accessible motor point, while muscles like tensor fascia latae and gluteus medius have two motor points. Muscles that are part of a larger region have a series of motor points. For example, the quadriceps have five and the hamstrings have seven motor points.
For decades, the approach for locating motor points was based on traditional measures. This is because the benchmark for locating motor points was based on acupuncture meridians whose point location was variable because the only measurement unit used was the cun – which is defined as the width of the patient’s thumb at the knuckle. The variability of this measurement from one subject to the next made this approach very difficult to reproduce during studies.
 |
|
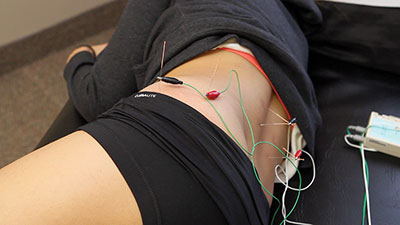
| Acupuncture or electroacupuncture can be used to restore motor function.
|
Then almost 40 years ago, researchers began measuring motor points using electronic equipment. Since then, several researchers have tried to make the mapping of motor points a reflection of some acupuncture points. However, the comparison of motor points and acupuncture points revealed that variability in locating motor points still exists because of inconsistency in the therapists’ ability to locate motor points.
Motor point locations are specific to a region of the muscle belly so the practitioner’s ability to stimulate the motor unit is not impaired, since motor points are actually located in areas of alpha-motor neuron accessibility – as opposed to an acupuncture point, which is more of a pin-point location.
Creating a simpler solution
Using this information I was able to create a simpler system for clinicians to follow. I developed a system for locating motor points by using a measurement most of us are familiar with: inches. Using inches along with anatomical reference points, I studied the early work of researchers Y. King Liu in 1975 and Ronald Melzack in 1977, and then I compared these studies to the more recent published pieces of Ja-Young Moon in 2012 and Alberto Botter in 2011. I was able to make a qualitative conversion in which the motor point mapping arrives at the same variable location as the research.
I was able to achieve and reproduce this system by converting cuns to inches. Many are unaware that the cun itself has a measured value of 1.312 inches. I simply took that value and began converting all traditional motor point mappings to a more familiar one.
Let’s take two motor points from the hamstring to illustrate how I simplify motor point location for the long and short head of the bicep femoris compared to methods described in the literature.
Long head biceps femoris:
- Take the halfway point between the centre of the popliteal fossa (BL40) and the centre of the ischial tuberosity.
- From this point, move one inch proximal and one inch lateral to arrive at the motor point.
Short head biceps femoris:
- Locate the centre of the popliteal fossa (BL39) and move one inch laterally.
- From this point, move six inches proximally to arrive at the motor point.
Putting it into practice
The benefits of using motor points during clinical treatments are plentiful when the goal of your treatment is to correct dysfunction and restore adaptability. Research demonstrates that very often, pain in one area of the body is a symptom for a weakness somewhere else.
In the Journal of Athletic Training, Phillip Gribble concluded that muscle groups in the proximal girdle of the kinetic chain of movement were associated with strength deficits in distal joint injuries.
Similarly, Bullock-Saxton, in the International Journal of Sports Medicine in 1994, noted the influence of distal joint injury on muscle activation of proximal muscles of the pelvic girdle. This research supports the use of a functional assessment system that encompasses the tissues involved around the centres of kinetic movement.
For example, non-traumatic knee pain can be a product of a motor inhibition of the hip abductors, while low back pain could be a consequence of inhibited rectus abdominus and oblique core musculature.
Once adopted by your practice, understanding and using this concept will produce quality clinical results to those patients with biomechanical dysfunction. Over the last decade researchers have discovered this and have come to the following conclusions:
Ingersoll (2003) in Rehab Management: “Without removing or reducing muscle inhibition, rehabilitation may essentially begin after healing occurs. We might also reduce long-term consequences associated with muscle inhibition, including susceptibility for further or other injury.”
Sedory (2007) in the Journal of Athletic Training: “Treatments that have been shown to reverse the effects of muscle inhibition should be used immediately before therapeutic exercise is performed in an effort to activate motor units that may have been previously inhibited.”
Nijs (2012), in the Clinical Journal of Pain: “Nociceptive motor inhibition might prevent effective motor retraining.”
If you have any questions or clinical observations, I can be reached through www.acupuncturemotorpoints.com and on Twitter @acupuncturepts.
Anthony Lombardi, DC, is consultant to athletes in the NFL, CFL and NHL, and founder of the Hamilton Back Clinic in Hamilton, Ont. He teaches his fundamental EXSTORE Assessment System and conducts practice-building workshops to health professionals. Visit www.exstore.ca for information.
This story was originally published in the December 2013 issue of Canadian Chiropractor [Web: 2013-12-05]
Print this page