
Laser Therapy: A guide for chiropractors
By Dr. Rick Ruegg BSc PhD DC and Jessica Wong
Features Clinical Techniques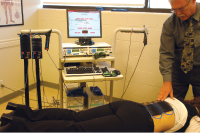 |
| BioFlex: the probe (LDI 200) has a 180 mW, 830nm GaAlAs LD. The cluster has 179 840nm SLDs delivering 1500 mW over 75 cm². |
Many health-care professionals are investigating the use of laser therapy on their patients, as they recognize its untapped potential in the treatment of musculoskeletal conditions. It has been more than 30 years since the initial reports on this form of therapy appeared, and, over time, studies have suggested its biological effects on injured tissue. With increasing research, as well as clinical utilization of laser therapy, chiropractors and students alike are curious about the efficacy of this treatment modality. However, questions regarding how laser therapy works, on a biological level, the indications for its use, and instrumentation parameters continue to be asked.
There are many elements of laser therapy that need to be explored before chiropractors and students can make an informed decision about this modality.
Low-level laser therapy (LLLT), commonly known as laser therapy or phototherapy, involves the application of light energy at specific wavelengths and power densities to penetrate into tissues and be absorbed by cells. The effect is not thermal, but instead related to photochemical reactions in the cells. These cumulative cellular benefits result in progressive improvements and sustained results. In comparison to other modalities, laser falls into the high-frequency (i.e., >10 000 Hz) range of modalities, much like ultrasound.
Low-to-medium-frequency (<10 000 Hz) modalities include TENS, EMS, microcurrent and IFC.
 |
| Med-X: the probe, has three LDs with a total power of 200 mW, the cluster has 49 633 and 870 nm SLDs delivering a total of 500mW of power. |
A number of research studies demonstrate the benefits of LLLT at a multitude of cellular levels. For instance, LLLT may play a role in stimulating growth factors and promoting angiogenesis at the vascular level, while helping stimulate T-cells and lymph nodes at the immune level. Also, early studies are showing the effects of decreased edema in the lymphatic system and increased stimulation of osteoclasts in bone. Overall, these cellular changes, induced by laser, provide temporary relief of muscle and joint pain and increase tissue healing. To appreciate why this occurs, an understanding of the physics and mechanisms of laser is necessary.
Superficial Laser Physics and Mechanism of Action
Laser therapy uses a form of electromagnetic radiation, which is energy that consists of photons travelling at the speed of light. Each photon carries energy in the form of a wave element, characterized by a specific wavelength and frequency. Photons of different wavelengths have different energy levels, which are organized into the “electromagnetic spectrum.” While this spectrum ranges from radio waves to gamma rays, for our purpose, the light used in laser therapy involves infrared, ultraviolet radiation and visible light. Specifically, LLLT has a therapeutic window between 630 nm and 1000 nm in wavelength.
A common question is “How can relatively weak electromagnetic radiation promote cellular changes?” Certain cell functions are stimulated by laser, especially those impaired by injury. Specifically, treated tissue has accumulated reactive oxygen species that influence ATP formation at a local level. Higher energy is not utilized because these levels of energy would become ionizing and damage the tissue.
Defining the Parameters for Laser Therapy
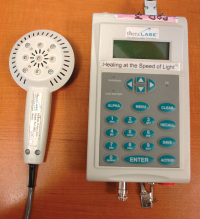 |
| Theralase: the probe has 5 X 100 mW LDs (905 nm) and 4 X 25 mW LDs (660 nm) for a total of 700 mW. |
Laser therapy remains a complex device to analyze, largely because it has a multitude of parameters that make it difficult to maintain homogeneity among research studies. However, it is still very important that LLLT parameters are well understood by health-care providers, as they greatly determine the laser’s effect on the condition being treated. In general, laser light has two main properties that differentiate it from a conventional light source: its narrow bandwidth and high degree of coherence. These parameters, among others, are defined and explained below:
Output Power: This determines the rate at which a given dose is delivered, and is measured in watts (W) or milliwatts (mW). Higher output power allows the desired dose to be delivered in shorter time duration. Therefore, higher power settings reduce the patient’s treatment time, while also delivering a higher amount of energy at a greater depth.
Power Density: This is the light
output power emitted per unit area of tissue illuminated by the laser light and is measured in mW/cm² or W/cm².
Dose: This represents the amount of energy delivered to a surface area of tissue, and is measured in Joules/cm². One Joule is equal to one Watt/second.
Duty Cycle: This is the amount of time the laser is delivering a dose during a given period of time. Essentially, this is used to describe a pulsed light source, which may vary between maximum (continuous emission) and zero (light source off). For example, if the duty cycle is 50 per cent, it indicates that the laser is on 50 per cent of the time. In relation to laser pulse, longer pulse duration causes an increase in the dose delivered to the patients, resulting in an increased duty cycle.
Superluminous Diodes Versus Laser Diodes: When comparing and contrasting the various laser devices available on the market, there are mainly two types of diodes used, which are superluminous diodes (SLD) and laser diodes. Lasers are monochromatic – i.e., producing light at a single wavelength – and are coherent – i.e., their waves are in phase. In contrast, SLDs produce a band of wavelengths, which spreads the light over a broad treatment area. The laser is also collimated, producing beams that are almost parallel with one another. This collimation increases the risk of eye damage if the light shines into one’s eyes. Furthermore, the true laser has a smaller spot size of around 3 mm² while SLDs are approximately 20 mm². In regards to power density, laser diodes have a greater power density (800-4,000 W/cm²) than SLD diodes (50-75 mW/cm²).
In summary, SLDs are selected for the treatment of a large surface area, as they are less powerful than laser diodes and rely upon a cluster of diodes to deliver a dose over a larger area. Laser diodes have higher power output and less divergent beam, making them suited as “laser probes” for deeper penetration over areas of localized pathology. In terms of coherence, research studies have shown that light with the same wavelength, intensity, and irradiation time produce the same biological effects, regardless of whether it is coherent or non-coherent. Therefore, the SLD would only require longer treatment times to match the dose delivered by a laser source.
Guide to Incorporating Laser into Practice
Enormous variations in the parameters reported throughout the literature make comparisons and conclusions very difficult. A literature review has assisted us in assessing this research. There are more than 2,500 published articles on LLLT, as well as 1,200 references in Tuner & Hode’s Laser Therapy Handbook. Among these articles, there are approximately 100 double-blinded studies. Upon review of this literature, the following treatment principles were identified:
Conditions Involving Soft Tissue: For acute soft tissue injuries, treatment should be initiated as early as possible, using low dosages of 4-8 J/cm² applied directly to the injury and other areas of palpable pain. Within the first three to four days after injury, frequency of care using this laser dose can be up to three times a day. There is no risk of harm to the patient, as this modality is non-thermal and would not enhance the inflammatory response. As the condition improves, the frequency of laser treatment may be reduced and dose increased up to 30 J/cm². It is important to note that since dose increases with longer pulse durations, initial treatments should use a low pulse rate of less than 100 Hz and later treatments can increase into the kilohertz range as the condition resolves. Overall, laser therapy can be very effective in accelerating the healing process for these types of injuries, allowing the patient to complete activities of daily living sooner.
Patients Presenting with Neurogenic Pain: With chronic neurogenic pain, LLLT is generally applied along the length of the affected nerves with a mid-range dose of 10-12 J/cm². Once again, this modality can be used on trigger points to desensitize the point to palpation. Areas of referred pain and corresponding dermatomes can also be treated for these patients.
Contraindications: It is important to note that contraindications to laser use include suspicious or cancerous lesions, pregnancy (relative contraindication), recent steroid injection sites, and direct use over the thyroid gland or eye area.
When it comes time for health-care providers to research the options and purchase a laser therapy device, there are many choices. It is important to remember that the power density of the unit will determine the treatment time for your patients and influence the suitability and practicality of the unit in your practice. The more user-catered properties of the devices, such as unit aesthetics and associated training and seminars, are unique to each company and allow practitioners to choose a device that most closely meets their needs. Overall, laser therapy can be a very powerful tool in the chiropractic toolbox. In Canada, laser therapy is beginning to make some small waves in the world of healing. With continued research and increased understanding of laser therapy, we believe that it will become one of the most effective healing modalities for our patients.
Bibliography:
Brosseau, L., Robinson, V., Wells, G., deBie, R., Gam, A., Harman, K., et. al. (2005). Low level laser therapy (Classes I, II and III) for treating rheumatoid arthritis. Cochrane Database of Systematic Reviews, Issue 4. Art. No.: CD002049. DOI: 10.1002/14651858.CD002049.pub2.
Fitz-Ritson, D. (2001). Lasers and their therapeutic applications in chiropractic. JCCA, 45(1):26–34.
Kitchen, S. (2002). Electrotherapy: Evidence-based practice (11th ed.). Melbourne, Churchill Livingstone.
Tuner, J. & Hode, L. (2004). The laser therapy handbook: A guide for research scientists, doctors, dentists, veterinarians and other interested parties within the medical field. Grangesberg: Prima Books.
Yousefi-Nooraie, R., Schonstein, E., Heidari, K., Rashidian, A., Akbari-Kamrani, M., Irani, S., et. al. (2007). Low level laser therapy for nonspecific low-back pain. Cochrane Data-base of Systematic Reviews, Issue 2. Art. No.: CD005107. DOI: 10.1002/14651858.CD005107.pub2.
 Dr. Rick Ruegg BSc, PhD, DC, is the Associate Dean of Clinics at the Canadian Memorial Chiropractic College. He can be reached at rruegg@cmcc.ca. Dr. Rick Ruegg BSc, PhD, DC, is the Associate Dean of Clinics at the Canadian Memorial Chiropractic College. He can be reached at rruegg@cmcc.ca. |
 |
Jessica Wong is a second-year student at CMCC. Having studied radiation therapy at the University of Toronto and the Michener Institute, she greatly understands the importance of interprofessional health care. She may be contacted at jjwong@cmcc.ca. |
Print this page