
It may seem contradictory to hear the term “healthy” inflammation;
however, inflammation is a key response of the body’s defence system –
a protective response involving cells and chemicals called to an area
to repair damage.
It may seem contradictory to hear the term “healthy” inflammation; however, inflammation is a key response of the body’s defence system – a protective response involving cells and chemicals called to an area to repair damage. Triggers that may cause inflammation include trauma such as fractures, sprains/strains, invading virus/bacteria, allergens, to list a few. Inflammation is an overall general innate response of the immune system to pathogens. Without inflammation, damaged tissue would not heal and further destruction would result.
Inflammation is typically noted by redness, swelling, heat, and pain, and is further defined as acute or chronic. It is when inflammation becomes ongoing, and the immune response is out of balance, that detrimental damage results in further tissue destruction, leading to the development of conditions such as allergy, arthritis, and autoimmune disorders. It is important again to note that the goal should not be to stop all inflammation, but to ensure that the balance of the immune response ensues.
A LOOK AT CYTOKINES
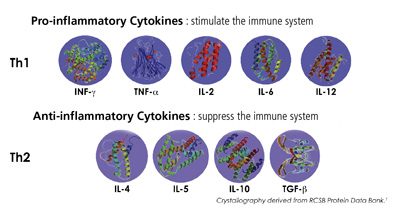
Cytokines are the key chemicals produced for cellular communication. These may be further subdivided into Th1 (pro-inflammatory) cytokines including INF-γ, TNF-α, IL-2, IL-6, and IL-12 and Th2 (anti-inflammatory) cytokines, which include IL-4, IL-5, IL-10, TGF-β (see figure 1). When Th1 cytokines predominate, acute inflammatory responses result, leading to uncontrolled tissue damage and autoimmune disorders. When Th2 cytokines are in excess, as seen in chronic inflammation, this may result in allergy and atopy (asthma, eczema, allergic rhinitis). There are many conditions in which markers of inflammation show this imbalanced state of Th1:Th2. The goal is to balance the Th1 and Th2 responses of the body, hence balancing the immune response and allowing the body to resume the normal inflammatory processes of repair and regeneration (see Figure 2).
 |
|
| Figure 1 – Pro- and anti-inflammatory cytokines.
|
|
 |
|
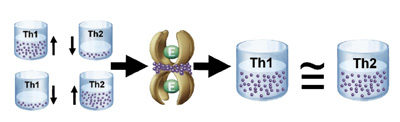
| Figure 2 – Systemic proteolytic enzymes can balance the Th1 and Th2 responses of the body.
|
SYSTEMIC ENZYME SUPPORT
The oral use of proteolytic enzymes, or proteases, from both plant (bromelain, papin) and animal (trypsin, chymotrypsin) origins, has been practised for decades and was originally studied by Dr. Max Wolf in the early 1930s.
Dr. Wolf created a very specific combination of these enzymes delivered along with rutin, which serves as a special
enteric coating to survive the acidic pH of the stomach. Proteases work by various means, including exposing antigenous epitopes, the degradation and removal of certain cytokines, the activation of receptors, and the proteolytic degradation of proteins damaged by inflammation and resulting in easier phagocytosis and removal.
Systemic proteases accelerate the clearance of cytokines and also assist in the elimination of immune complexes and amyloid polymers such as those seen in Alzheimer’s disease.
When cytokines are restored to a balanced state, the immune system is able to function optimally, reducing pain and tissue damage, and restoring function. A recent study on rotator cuff tendinitis demonstrated an improvement in both pain and disability in the group receiving system enzyme support along with other naturopathic modalities. Another study using systemic enzyme support in rheumatoid arthritis resulted in improvement not only in the Ritchie Index, morning stiffness, and the Lee index, but serum concentrations of pro-inflammatory cytokines were significantly reduced in the enzyme group compared to the control group. The group receiving systemic enzyme support showed a significant decrease in exudative exacerbation within three to five days of treatment. There was also a normalization of biochemical and immunological parameters seen in this group. Another condition known to have an inflammatory component and immune imbalance is psoriasis.
FOODS AND THE INFLAMMATORY RESPONSE
As with any health strategy, that which we put into our body will affect its ability to heal and repair. A diet consisting of foods that reduce inflammation should include essential fatty acids from fish and nuts, the spice turmeric, and antioxidants from vegetables and fruits: all may assist in keeping inflammation low.
Foods that may trigger inflammation should be reduced or eliminated from the diet. These may include those foods containing the alkaloid solanine found in the nightshade family (peppers, tomatoes, potato, and eggplant) and those high in arachidonic acid (meats, eggs). Eliminating refined sugars, white flours, processed foods including those with nitrates – as they may perpetuate a rise in inflammatory mediators – is also highly recommended. Another consideration is removing gluten, which can contribute significantly to inflammation, from the diet. Gluten sensitivity is now being recognized as far more prevalent than previously thought and testing is available to identify those who are sensitive.
Although systemic enzyme support may consist of the same proteolytic enzymes as enzymes that are used to support digestion, their intent is to reach the systemic circulation. It is imperative, then, that they are used on an empty stomach (45 minutes prior to eating or several hours after food) in order to achieve this desired effect.
It is apparent that a healthy immune response to injury/trauma involves an inflammatory response. When this response is balanced and appropriate, the body will heal and move to a state of recovery quickly and without complication. When this process is out of balance, pain, reduced healing, and chronic inflammatory conditions may result. Systemic enzyme support assists the body in reaching balance more readily with minimal to no side-effects, unlike some traditional pharmaceutical treatments.
For more details on the pharmacokinetic effects of or further research on systemic enzyme support, please visit www.systemicenzyme.org .
Dr. Victoria Coleman is a 1994 graduate of CMCC and a BSc in Kinesiology specializing in Fitness Assessment and Exercise Counseling. Working with patients over the years, it became her mission to teach people that everything you eat, breath, drink, and think affects your health. This fuelled her desire to further expand her career and continue her studies. She is an avid follower of the Institute for Functional Medicine and is currently working toward her certification in Functional Medicine. Dr. Victoria Coleman is also the president of Douglas Laboratories/Pure Encapsulations Canada.
Print this page