Mineral matters
By Richard Danel
Features Nutrition WellnessAddressing magnesium deficiency in patient population and exploring more effective means of administration
Magnesium is considered one of the three essentials of life, together with water and oxygen. It is the most important mineral for our body, required by more than 327 known enzymatic processes. It regulates everything from basic metabolism, hormones and sleep to healthy blood pressure and bone formation.
A healthy magnesium balance helps prevent conditions like cardiovascular disease and stroke, type 2 diabetes, osteoporosis, certain cancers and migraine headaches, and alleviates existing problems like muscle cramps and aches, restless legs, insomnia and anxiety.
Probably more than 70 per cent of western society is deficient in this mineral – even those who eat lots of green vegetables, grains, nuts, beans and other magnesium-rich foods. This is because since the introduction of modern agriculture, soils got depleted of magnesium, so vegetables aren’t getting enough anymore. Modern food processing also causes significant loss of magnesium.
In addition, our modern, stressful lifestyle demands higher magnesium intake – like the extra gas your car needs in a high-speed chase.
Healthy balance
A 2009 report from the World Health Organization estimated that 75 per cent of adults consume a diet deficient in magnesium. In western society, restoring and maintaining a healthy magnesium balance is virtually impossible without supplementation.
Even if one limits foods to those that are relatively rich in magnesium, there’s another crucial factor: the magnesium/calcium ratio (Mg/Ca). While there is still discussion about the ideal ratio, varying from 2Mg/1Ca to 4Mg/1Ca, the current Mg/Ca ratio in our diet is 1Mg/5Ca on average, which is too high a ratio for calcium.
Unfortunately, the magnesium-rich ingredients we’d like to be picky about will also elevate the calcium intake and hence not improve our magnesium balance as we want.
According to recent research, milk and other dairy products may contain too much calcium, which has been linked to problems with bone formation in children, fractures in adults and even higher mortality.
Recent publications also show the correlation between consumption of red meat and processed meat on one hand, and the increased risk of colorectal cancer on the other hand. Magnesium deficiency also increases the risk of colorectal cancer. Further research must bring clarity on the role of magnesium in our dairy- and meat-rich diet.
Magnesium is one of seven nutrients placed on the U.S. Department of Health’s list of nutrients of concern, published as part of its Dietary Guidelines for Americans. To explore which form of magnesium supplementation is ideal, we need to distinguish three things: recommended intakes; magnesium compounds; and routes of administration.
Recommended intakes
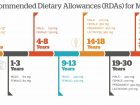
Intake recommendations for magnesium and other nutrients are provided in the Dietary Reference Intakes (DRIs) developed by the U.S. Food and Nutrition Board (FNB) at the Institute of Medicine, National Academies (formerly, National Academy of Sciences). DRI is the general term for a set of reference values used to plan and assess nutrient intakes of healthy people. These values, which vary by age and sex, include:
- Recommended dietary allowance (RDA) – the average daily level of intake sufficient to meet the nutrient requirements of nearly all (97 to 98 per cent) healthy individuals.
- Adequate intake (AI) – established when evidence is insufficient to develop a RDA and is set at a level assumed to ensure nutritional adequacy.
- Estimated average requirement (EAR) – average daily level of intake estimated to meet the requirements of 50 per cent of healthy individuals.
- Tolerable upper intake level (UL) – maximum daily intake unlikely to cause adverse health effects.
Magnesium compounds
Magnesium supplements are available in a variety of compounds, including magnesium chloride, citrate, sulphate and oxide. Many supplement labels do not declare the amount of elemental magnesium, but the weight of the entire magnesium-containing compound.
Absorption of magnesium from different kinds of magnesium supplements varies substantially. Forms of magnesium that dissolve well in water are absorbed better in the intestine than less soluble forms. Studies have found that magnesium in chloride form has a superb bioavailability and less adverse effects than in sulfate form, for instance.
Many researchers advocate magnesium chloride as the most effective and most natural form of dietary supplementation, in part due to the chloride’s natural occurrence in hydrochloric acid in the stomach.
Routes of administration
There are four main routes for magnesium to reach our cells: intravenously, pulmonary uptake, orally and transdermal uptake.
Intravenous and pulmonary uptake, though both effective in their own employments, demand (almost) clinical conditions, like hygienic measures, that narrow the window of applications.
An interesting development in recent times is the increasing trend toward transdermal administration. Considering that oral administration of magnesium has its limitations in terms of poor bioavailability and unwanted intestinal effects, transdermal administration of magnesium chloride could be a very welcome new avenue in helping western society cope with magnesium deficiency.
Though still controversial, worldwide anecdotal evidence justifies further scientific exploration of the effectiveness of the transdermal route. But let’s dig a little deeper into this increasingly utilized method of magnesium administration.
Magnesium chloride dissolved in water has the highest possible concentration (31 to 33 per cent) of magnesium. Because of the extreme high concentration, the assumption is that magnesium penetrates the skin barrier and cell junctions and reaches in succession the interstitial space, the fluid surrounding all of our cells, becoming rapidly and completely available as free elemental magnesium without any intestinal effect.
Hypothesis
In talking with some of the world’s top magnesiologists, the following hypothesis came up to possibly explain the increasing evidence of transdermal effects of topically applied magnesium.
Step 1. What we know
It is known that during urine production, something special is going on in our kidneys with magnesium: like many other ions, magnesium is abundantly excreted initially during urine production. In the further course of urine output many valuable components are regained. But in the so-called distal tubules of the nephrons, just before final urine output, there are cells especially dedicated to actively re-absorb magnesium – and it’s not only by osmosis, diffusion, e-potential, or other non-energy consuming processes. Those cells really actively re-absorb magnesium all the way through their membranes and cell content. It costs energy, but they just do it in order to protect the body for magnesium loss.
Step 2. The assumption
Another way to lose minerals, including valuable magnesium, is through sweating. Because sweat production has similarities with urine production, it would not be surprising if Mother Nature provided sweat glands with a somehow similar magnesium re-absorption mechanism. Actually, there is growing scientific evidence for this assumption, such as studies by Thomas Jentsch et al. of the physiological function of the chloride channels in sweat glands (2002, American Physical Society).
Step 3. Here’s the catch
Magnesium oil applied on the skin or magnesium chloride in a bath brings magnesium ions into the distal part of sweat glands. When the ‘actively re-absorbing magnesium-cells’ detect a high concentration of magnesium, they will just do their job and re-absorb magnesium; even if it’s coming from outside. This is the transdermal uptake.
Dr. Richard Danel, MD, is chairman of Magnesium Health Institute, with offices in Vancouver and The Netherlands. The Magenesium Health Institute studies the improvement of magnesium balance and the role magnesium plays in healthy ageing. Contact him via his website: www.magnesiumhealthinstitute.com or visit imagnesium.com for more information.
Print this page