
Regenerative injection therapy: The use of dextrose and mannitol injections for the treatment of chronic pain
By Dr. Chris Spooner, ND
Features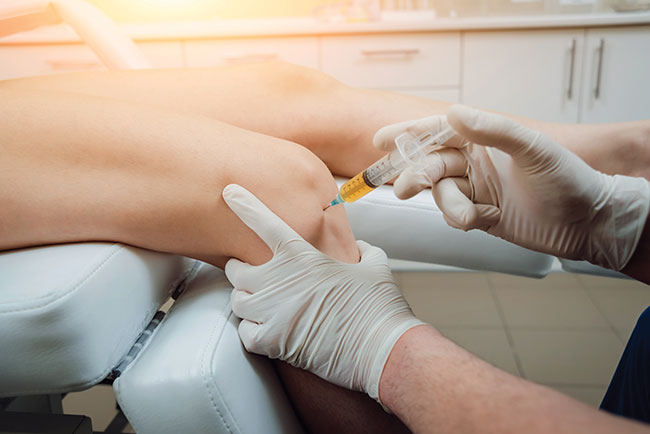 Recent basic science and clinical research suggest several ways ways in which dextrose can reduce pain, improve overall function, and more. Photo credit: © romaset / Adobe Stock
Recent basic science and clinical research suggest several ways ways in which dextrose can reduce pain, improve overall function, and more. Photo credit: © romaset / Adobe Stock
Musculoskeletal conditions are common in men and women of all ages across all socio-demographic strata of society. They are the most common cause of severe long-term pain and physical disability and affect hundreds of millions of people around the world. The impact on all aspects of life through pain and by limiting activities of daily living typically by affecting dexterity and mobility.i
Many musculoskeletal conditions are nonspecific with no defined tissue-based cause and, although they may have a low level of associated disability, they are extremely common. The prevalence of chronic pain and the challenges in treatment have been responsible for an opioid epidemic that has resulted in a national crisis of opioid-related deaths. Other harms associated with treatment, including medication-based interventions (notably long-term, corticosteroids, and nonsteroidal and immunosuppressive therapies) and surgical interventions, are not captured in the estimation of burden.ii
National organizations have called for new therapies to treat chronic pain, including therapy that addresses the underlying pain pathology. An overarching goal is to produce improved non-opioid treatment regimens.
The focus is this article is a discussion of the evidence base underpinning the therapeutic injection of dextrose, an agent used in several emerging, distinct but related injection-based modalities, prolotherapy and perineural injection therapy. Recent basic science and clinical research suggest several ways in which dextrose can reduce pain, improve overall function and restore connective tissue function.
Many drugs try to tame inflammation by inhibiting molecular events occurring at the beginning of the immune response. However, rather than blocking inflammation in the bud –which may thwart the body’s own attempt to heal – a better approach may be to enhance the activity of these natural resolution-promoting compounds.
The initial inflammatory responses involve the release of compounds known to incite inflammation, leukotriene B4 (LTB4), followed by prostaglandin E2 (PGE2) which is the target of NSAIDs. However, this is then followed by the production of an anti-inflammatory compound, lipoxin A4 (LXA4). This results in the reduction of inflammatory cells at the site of injury and inflammation eventually resolves. It turns out that PGE2, thought to incite inflammation, is doing the opposite and initiates the production of the anti-inflammatory LXA4 setting the stage for resolution.
What is Prolotherapy?
The goal of prolotherapy is to repair weakened or stretched ligaments or tendons or stabilize joint surfaces affected by arthritis. Dextrose injection (12.5% to 25% concentration) stimulates a brief arachidonic acid (AA) pathway inflammation that involves leukotriene B4 (LTB4), followed by prostaglandin E2 (PGE2). This can seem contradictory as this inflammation is the type of inflammation to which most doctors are referring when they use that word. As noted above, after an injury, the body uses primarily AA inflammation to try to repair the damage via the production of an anti-inflammatory compound, lipoxin A4 (LXA4). This results in the reduction of inflammatory cells at the site of injury and inflammation eventually resolves.
Injuries, such as a sprained ligament, a twisted knee, whiplash, or repetitive movements can tear or fray these cable-like structures of ligaments and tendons. The injury typically causes some local inflammation, and the repair process is initiated. If the healing process is completely successful, the ligaments or tendons will be restored to their normal strength and length, and you can return to your normal activities. If this healing process does not completely work, the ligaments or tendons may remain in a stretched or weakened state. This “stretched out condition may cause pain and discomfort with movement or result in joint instability. Chronic ligament or tendon damage also can cause the surrounding muscles to tighten up and cause additional pain.
In chronic damage, there is a disruption of the normal parallel arrangement of the collagen fibres.iii, iv Persistently injured ligaments and tendons may have 30-40% fewer collagen fibres, and the fibres are in disarray or unorganized.
Electron microscopic studies have demonstrated that degenerative ligaments and tendons do not contain cells of inflammation. Studies have shown that sometime between 4-10 weeks after a tendon or ligament injury, there is no longer inflammation present. The resulting ligament or tendon is degenerated, weakened, and overstretched. Pain is still experienced, not because of inflammation, but because of the degenerative process.
With prolotherapy, there is no significant damage, because there is no stretching or tearing of fibres, but the body still begins a repair process, which allows the structure to become stronger and tighter rather than first becoming weaker and looser. Unlike injections of corticosteroids, which also suppress inflammation and provide only temporary relief for a chronic condition, prolotherapy injections given over several months are meant to provide a permanent benefit. In effect, prolotherapy tricks the body into initiating a healing response.
The technique reactivates the healing process by injecting a mildly irritating substance – commonly a somewhat concentrated sugar solution along with the painkiller procaine or lidocaine – into the injured area to stimulate a temporary low-grade inflammation. In some cases, growth factors themselves may be injected.
With growth factors in place at the site of inflammation, new tissue is said to be produced that strengthens lax or unstable ligaments and tendons. The technique may even support damaged or degenerated cartilage, which normally does not repair itself, by strengthening the fibrous connective tissues that stabilize the area.
Several excellent studies published in the last few years in respected specialty journals have shown beneficial results to prolotherapy.v, vi, vii, viii In addition, the Mayo Clinic Health Letter spoke positively about prolotherapy and its future.ix The clinic stated that when chronic ligament or tendon pain fails to respond to more conservative treatments like physical therapy and prescribed exercises, “prolotherapy may be helpful.”
There have been two review articles recently published indicating significant benefits from prolotherapy and chapters are included in two newly published pain management textbooks.x, xi, xii, xiii
Prolotherapy has proved incredibly helpful for addressing musculoskeletal pain for several reasons:
- It is safe, comparable to the safety of acupuncture if physicians have been fully training in needle placement methods.xiv
- It uses very low cost and readily available sterile dextrose
solutions. - It can be used to treat complex cases that require treatment of many areas simultaneously for benefit.
- Dextrose has a proven ability to grow normal ligament tissue.xv, xvi, xvii, xviii
- Dextrose has a unique analgesic effect that occurs in seconds without an anesthetic. xix, xx
- Dextrose has been shown to stimulate some cartilage cell growth. Note, this does not resurface joints, but the goal is to stabilize and calm the joint surface in arthritis.xxi
In clinical practice, I have found that judiciously combining prolotherapy with other modalities, such as chiropractic, active release technique, massage and physiotherapy, results in a more comprehensive treatment approach in which the entire source of pain is completely identified and treated.
PIT and how it works
Another injection therapy that has proven useful is Perineural Injection Therapy (PIT). PIT is the injection of isotonic dextrose or mannitol close to superficial, subcutaneous nerves to restore normal function in nerves that cause chronic pain and degeneration. Treating with a combination of prolotherapy and perineural injection simultaneously addresses nerve, ligament, tendon, muscle, and joint sources of pain.
There is another type of inflammation that has been recognized, neurogenic inflammation. This type of inflammation is produced by special small sensory nerves that are protein-producing (“peptidergic”). Neurogenic inflammation occurs when a nerve produces painful or damaging proteins. The receptor that is involved is TRPV-1 (transient receptor potential vanilloid – Type 1) also known as the capsaicin receptor, which plays a central role in the development of allodynia and hyperalgesia in patients with chronic pain.xxii, xxiii
Chronic neuropathic pain is associated with persistent upregulation of the TRPV1 ion channel. Studies suggest a potential nerve-specific or sensorineural mechanism for pain reduction following perineural injection of isotonic 5% dextrose
(D5W)xxv Dextrose acts at the level of the TRPV1 receptor. Mannitol, a metabolically inert sugar molecule that is structurally similar to dextrose, has been reported to reduce pain resulting from upregulation of TRPV1 ion channels in an RCT using a capsaicin pain model.xxv
TRPV-1 nerves are not only irritated when they have to penetrate fascia at the skin level, but also when they have to penetrate layers of fascia in other regions, such as fibro-osseus tunnels, or passages. Any of these areas can malfunction or be changed in such a way as to “touch” the TRPV -1 nerve.
Perineural injections use 5% dextrose water (D5W) as a fluid injection under pressure to purposely separate nerves from areas of suspected fascial compression, which are increasingly viewed as potential perpetuating factors in recalcitrant neuropathic pain/complex regional pain. The mechanism of analgesia may be related to an indirect (allosteric) effect on the TRPV1 cation channel, and the injection of D5W results in a release of the fascial compression of a suspected local neural compression. This addresses chronic constriction injury which contributes to neuropathic pain and neural swelling.xxvi
The judicious use of prolotherapy and perineural injections can be an important element of a comprehensive, holistic treatment plan to address structural and neural aspects of chronic pain. The proliferative properties of hypertonic dextrose can facilitate tissue repair via arachidonic acid pathways, leading to the resolution of chronic ligamentous and tendonous pain. Perineural injection with isotonic dextrose or mannitol can address neuropathic pain that is a driver of chronic pain. The down-regulation of the TRPV-1 receptor re-establishes neuronal function and results in a return to normal innervation that improves pain and function.
Both of these therapies are without the harms associated with medication-based interventions such as long-term opioid use, corticosteroids, nonsteroidal and immunosuppressive therapies and surgical interventions by addressing the underlying pain pathology.
REFERENCES
- i Woolf AD, Erwin J, March L. The need to address the burden of musculoskeletal conditions. Best Pract Res Clin Rheumatol. 2012 Apr;26(2):183-224. doi: 10.1016/j.berh.2012.03.005. PMID: 22794094.
- ii Fiona M. Blyth, Andrew M. Briggs, Carmen Huckel Schneider, Damian G. Hoy, and Lyn M. March 2019:
- The Global Burden of Musculoskeletal Pain—Where to From Here? American Journal of Public Health 109, 35_40, https://doi.org/10.2105/AJPH.2018.304747
- iii Frank C. The Pathophysiology of Ligaments. Chapter 2:11-18. In: Arendt EA. Orthopedic Knowledge Update: Sports Medicine 2, American Academy of Orthopedic Surgeons, 1999.
- iv Rodeo SA, Izawa K. Pathophysiology of Tendinous Tissue. Chapter 4: 29-36. In: Arendt EA. Orthopedic Knowledge
- Update: Sports Medicine 2, American Academy of Orthopedic Surgeons, 1999.Cyriax, J. Textbook of Orthopedic Medicine, Bailliere Tindall, London, 1982.
- v Topol, Gaston A,MD, Reeves, K. Dean, MD, Hassanein, K.M, PhD., “Efficacy of Dextrose Prolotherapy in Elite Male Kicking-Sport Athletes with Chronic Groin Pain”, Arch Phys Med Rehabil , Vol 86, April 2005.
- vi Ohberg, Lars, Alfredson, H, “Sclerosing Therapy in Chronic Achilles Tendon Insertional Pain—Results of a Pilot Study”, Knee Surg Sports Traumatol Arthrosc, (2003) 11:pp.339-343.
- vii Centeno, Christopher, MD, Elliott, James, MSPT, et. Al, “Fluoroscopically Guided Cervical Prolotherapy for Instability with Blinded Pre and Post Radiographic Reading”, Pain Physician, 2005;8:67-72.
- viii Wilkinson, Harold, MD, PhD. ‘Injection Therapy for Enthesopathies Causing Axial Spine Pain and ‘The Failed Back Syndrome:’ A Single Blinded, Randomized and Cross-Over Study”, Pain Physician, 2005;8:167-173.
- ix Mayo Clinic Health Letter, Volume 23, Number 4, April 2005
- x Dagenais, Simon, DC, PhD., Haldeman, Scott, DC, MD, Wooley, J, DC, “Intraligamentous Injection of Sclerosing Solutions (Prolotherapy) for Spinal Pain: A Critical Review of the Literature”, The Spine Journal 5 (2005) 310-328.
- xi Rabago, David, MD, Best, Thomas, MD, et. al, A systematic Review of Prolotherapy for Chronic Musculoskeletal Pain”, Clinical Journal of Sports Medicine, Vol 15, Number 5, September 2005.
- xii Linetsky, Felix, MD., Miguel, R, MD, Saberski, L., MD, “Pain Management with Regenerative Injection Therapy (RIT), Pain Management, A Practical Guide for Clinicians, Sixth Edition, American Academy of Pain Management, CRC Press, 2002, pp. 381-402
- xiii Linetsky, Felix, MD, Eek, B, MD, Derby, R, MD, Parris, C.V.W., MD, “Regenerative Injection Therapy”, Low Back Pain, Diagnosis and Treatment, Interventional Pain Management, ASIPP Publishing, 2002, pp. 519-540.Chronic pain
- xiv Martins et al. Martins CA, Bertuzzi RT, Tisot RA, et al. Dextrose prolotherapy and corticosteroid injection into rat Achilles tendon. Knee Surg Sports Traumatol Arthrosc 2012;20:1895-900.
- xv Oh S, Ettema AM, Zhao C, et al. Dextrose-induced subsynovial connective tissue fibrosis in the rabbit carpal tunnel: A potential model to study carpal tunnel syndrome? Hand (N Y). 2008;3(1):34-40.
- xvi Yoshii Y, Zhao C, Schmelzer JD, et al. The effects of hypertonic dextrose injection on connective tissue and nerve conduction through the rabbit carpal tunnel. Arch Phys Med Rehabil 2009;90:333-9
- xvii Yoshii Y, Zhao C, Schmelzer JD, et al. Effects of hypertonic dextrose injections in the rabbit carpal tunnel. J Orthop Res 2011;29:1022-7
- xviii Yoshii Y, Zhao C, Schmelzer JD, et al. Effects of multiple injections of hypertonic dextrose in the rabbit carpal tunnel: a potential model of carpal tunnel syndrome development. Hand (N Y) 2014;9:52-7
- xix Maniquis-Smigel L, Reeves KD, Rosen JH, et al. Short term analgesic effects of 5% dextrose epidural injection for chronic low back pain. A randomized controlled trial. Anesth Pain Med. 2017;7(1):e42550.
- xx Maniquis-Smigel L, Reeves KD, Rosen JH, et al. Analgesic effect and potential cumulative benefit from caudal epidural D5W in consecutive participants with chronic low back and buttock/leg pain. Jnl Alt Compl Med. 2018
- xxi Topol GA, Podesta LA, Reeves KD, et al. The chondrogenic effect of intra-articular hypertonic-dextrose (prolotherapy) in severe knee osteoarthritis. PMR. 2016;8(11):1072-1082.
- xxii Basbaum AI, Bautista DM, Scherrer G, Julius D. Cellular and Molecular Mechanisms of Pain. Cell. 2009;139(2):267-284.
- xxiii Cui M, Gosu V, Basith S, et al. Polymodal Transient Receptor Potential Vanilloid Type 1 Nocisensor: Structure, Modulators, and Therapeutic Applications. Adv Protein Chem Struct Biol. 2016;104:81-125.
- xxiv Wu P, Diaz R, Borg-Stein J. Platelet-Rich Plasma. Phys Med Rehabil Clin N Am. 2016;27(4):825-853.
- xxv Bertrand H, Kyriazis M, Reeves KD, et al. Mannitol cream in the treatment of postherpetic neuralgia: Randomized, placebo-controlled, crossover pilot study (Abs). Can Fam Physician. 2017;63(Suppl 1):S106.
- xxvi Lam SKH, Reeves KD, Chang AL. Transition from deep regional blocks toward deep nerve hydrodissection in the upper body and torso. Method description and results from a retrospective chart review of the analgesic effect of 5% dextrose water as the primary hydrodissection injectate. Biomed Res Int 2017;7920438 (doi.org/10.1155/2017/7920438).
Dr. Chris Spooner ND, B.Sc. is a North Okanagan naturopathic doctor with 20 years of clinical experience. In his private practice, Paradigm Integrative Medicine, Dr. Spooner works with patients looking for a balanced approach to health care that combines conventional medicine with research informed integrative approaches. Dr. Spooner has advanced certifications through the College of Naturopathic Physicians of B.C., including prescriptive authority. He has been a board member and vice chair of the College of Naturopathic Physicians of British Columbia since 2008.
Print this page