Virtually every symptom and condition that a chiropractor encounters in a clinical setting has an inflammatory component.
Virtually every symptom and condition that a chiropractor encounters in a clinical setting has an inflammatory component. Whether the individual presents with a recurring chronic condition, an acute injury, degenerative changes, an arthritic condition, headaches, autoimmune disease, insulin resistance, joint dysfunction, or subluxation, inflammation is a part of the process underlying their condition.
 |
|
| Suggest your patients add protein to every meal. Protein has high satiation value and rich in nutrients. Photo: Fotolia Advertisement
|
In order to promote pain relief and healing, managing inflammation is critical. Controlling systemic inflammation is especially important in the management of chronic conditions. It is also important during the proliferation, remodeling and repair phases of healing following an acute injury, in order to prevent progression to a chronic pain condition.
A growing body of literature is showing that nutrition intervention is an effective tool for regulating systemic inflammation.
Before we get into specific recommendations, let us look at why it is likely that most (if not all) of the patients we see in our offices have chronic systemic inflammation.
Diet debacle
The Standard North American Diet (SNAD) includes consumption of large amounts of sugar, highly processed carbohydrates, highly processed industrial fats (trans fats, seed and vegetable oils), gluten and conventionally raised, confinement-operation meat products.
 |
|
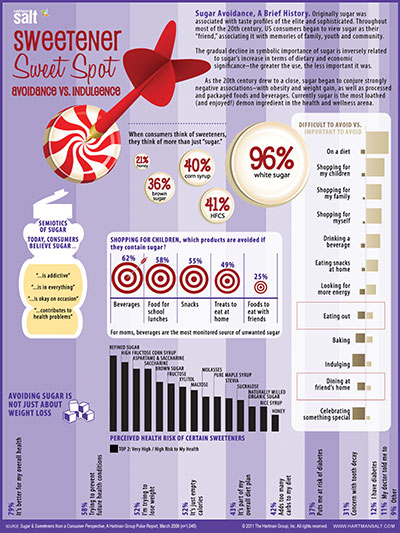
| Info graph: The Hartman Group
|
This diet contains an excessive amount of omega-6 fatty acids. Omega-6 fats form the precursors for pro-inflammatory eicosanoids. High omega-6 status – especially when combined with poor omega-3 status – causes an excessively high inflammatory response to normal stimuli.
Another problem with the SNAD diet is that it is insufficient in omega-3 fatty acids. Omega-3 fats form the precursors for anti-inflammatory eicosanoids. Poor omega-3 status prevents production of anti-inflammatory eicosanoids and leads to an exaggerated and prolonged inflammatory
response to normal stimuli.
An ideal ratio of omega-6 to omega-3 fatty acids in the body is 1:1. Due to the massive consumption of canola and soy oil in modern foods, as well as the changes in the fat profile of livestock fed with grain and raised under stressful conditions, current estimates of the omega-6 to omega-3 tissue ratio for most people ranges from 10:1 to 20:1 – with a ratio as high as 25:1 in some individuals.
The SNAD diet is also lacking in organ meats and fermented foods. As a result, most people are not consuming sufficient levels of the valuable nutrients found abundantly in these foods. These include fat soluble vitamins (A, D, E, K and K2), iron, B vitamins and probiotic cultures.
Other important factors that are strongly linked to elevated inflammatory markers are lack of movement (sedentary lifestyle), poor sleep, chronic psychological and emotional stress, and poor gut health.
Baby steps
Looking at this laundry list of dietary missteps and other lifestyle factors that are elevating the inflammatory response and exacerbating a person’s condition can feel a bit overwhelming. This is not to suggest that you list off all of these things to any one patient and tell them that they have to change them all.
While it may be better for them to do a complete overhaul, this is a process that is better taken in baby steps. They will only benefit from the advice that they put into action.
In order to have high compliance and actually make an impact, it is best to start by adding, rather than taking away. Instead of telling patients to stop eating all of their favourite foods, make a suggestion to pick one healthy item to add to their diet on a daily basis (or other consistent schedule).
For example, a great place to start would be to add a high-quality omega-3 supplement daily or omega-3 rich foods (salmon, shell fish, sardines, spirulina/algae) three times a week. This first step can go a long way toward balancing their omega-6 to omega-3 ratio and can drastically improve their immune function and inflammatory status.
Once they are consistently following your first recommendation, additional great foods to add to any diet would be 5,000 IUs of vitamin D daily, and a high-quality, multi-strain probiotic supplement or fermented, unpasteurized probiotic foods (such as pickles, sauerkraut, kim chi, kefir, plain yogurt and kombucha).
These simple dietary changes can massively impact healing and chronic pain symptoms.
For individuals who are significantly overweight, decreasing inflammation alone has been shown to improve their ability to lose body fat and decrease joint pain.
 |
Making the change
If you think a patient is ready to begin taking bigger steps toward changing his or her diet for the better, the following are dietary recommendations that are easy to communicate and easy for patients to follow successfully.
- Have protein every time you eat. Protein has high satiation value and all whole food protein sources are nutrient dense (meat, eggs, seafood, algae, nuts).
- Eat simple meals. The best meals consist of protein – like meat or fish – plenty of non-starchy vegetables, whole food carbohydrates from root vegetables or fruit, and some healthy fat.
- Focus on food quality. Get the best-quality meats, vegetables, fruits, nuts and seed and fats that your budget will allow. Higher-quality food contains fewer toxins and will be less inflammatory.
- Do not try to restrict portion sizes. This is especially important at the very beginning of the process. When people are transitioning to eating a healthier diet, eating to satisfaction is positive reinforcement and will make the transition smoother and more rewarding. Additionally, food restriction can lead to depriving the body of the calories and nutrients it needs to function optimally, causing additional stress.
While most of the people in your office may not have come to you expecting dietary advice, subtle changes in their nutrition status can have a massive impact on the results that they have under your care, and their overall health and well-being.
As a knowledgeable health-care provider, making these types of recommendations can improve patient outcomes, increase levels of satisfaction and allow you to build excellent rapport with the people in your community.
If you are going to make dietary recommendations, it is helpful to provide additional resources for people. Research local health food stores, farmers’ markets, local farms that pasture-raise their hormone- and antibiotic-free animals, organic community shared agriculture programs, and healthy restaurants in your area so that you can point people in the right direction.
You may also consider recommending or retailing certain high quality brands of different supplements.
Fish oil brands I commonly recommend include: Green Pastures Cold Fermented Cod Liver Oil, Natural Factors, NutraSea and BonFire.
Probiotic brands I commonly recommend include: Progressive HCP 30 or HCP 70, CanPrev Pro-Biotik 15B, and Flora Udo’s Choice.
Vitamin D brands I commonly recommend include: CanPrev D3 Drops and Orange Naturals D3 + K2 drops.
These are just a few that I have looked into and feel comfortable recommending to my patients, but there are many other great-quality brands out there that will work well for your patients.
One last thought: If patient nutrition is not an area of expertise or passion for you, consider teaming up with a local nutritionist who will do a good job of supporting anyone that you send to them.
Having a healthy diet is an essential part of living well; it is an exciting and rewarding way to support the people that we care for.
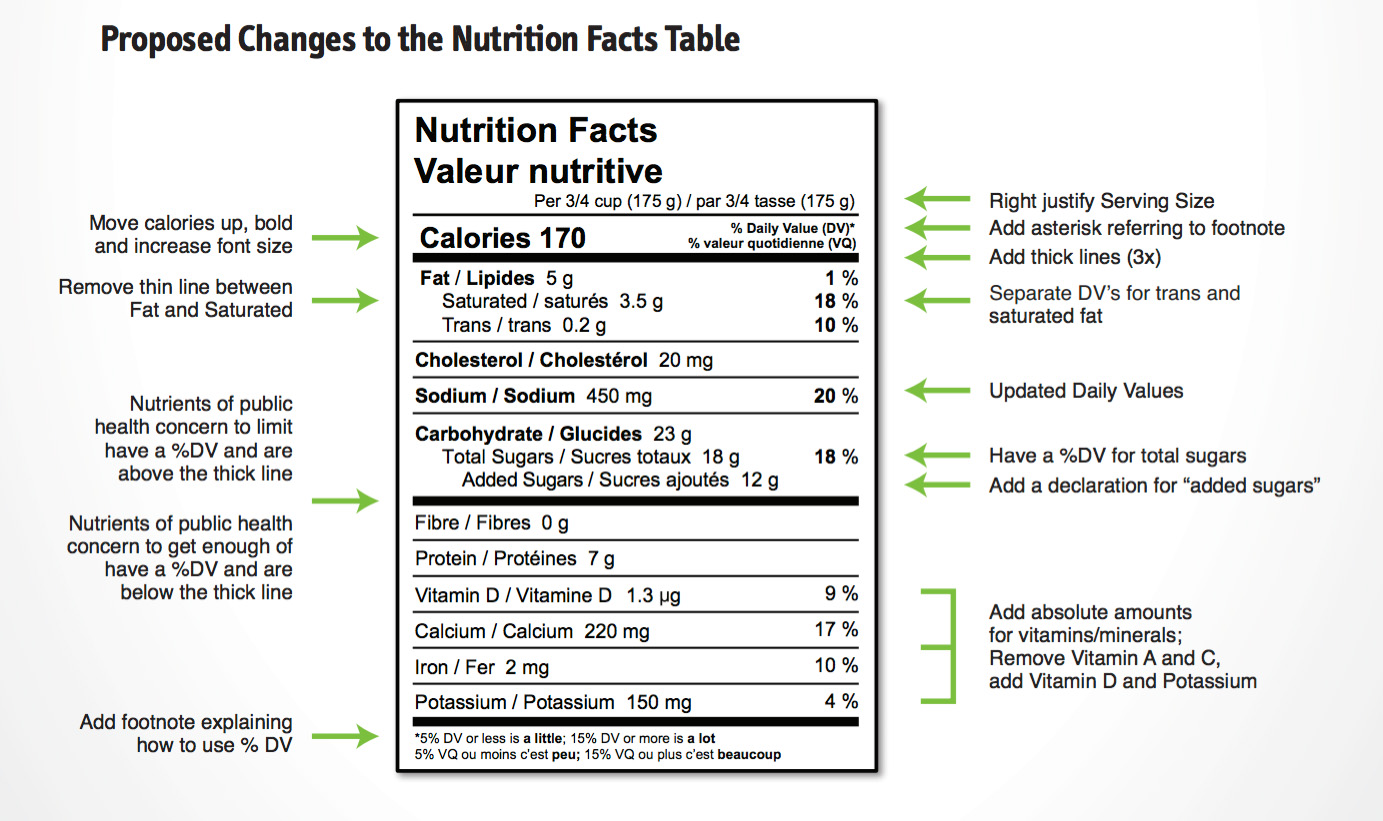
| FACT CHECK – WHAT’S IN THE FOOD? Health Canada is proposing to update the Nutrition Facts table for prepackaged foods to reflect the latest scientific information, as well as changing the look of the Nutrition Facts table and the list of ingredients so that they can best help Canadians make informed choices when selecting foods for themselves and their families. Some of the proposed changes to the Nutrition Facts table include:
*Source: Health Canada |
 |
|
Dr. Justine Ward, D.C., has a family wellness practice in London, Ont. In her practice, she places special emphasis on care for families trying to conceive, pregnancy, childbirth, babies and raising healthy families. She believes in empowering everyone she meets to achieve their full potential.
Print this page