
Trigenics® as an effective complementary tool.
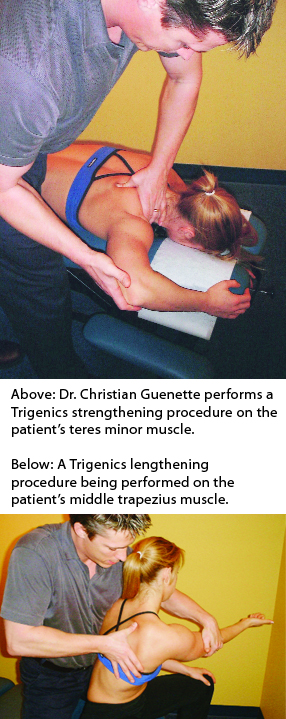 Trigenics®, developed in the early 1990s, is referred to by its founder, chiropractor Dr. Allan Oolo Austin, as an interactive neurological treatment system. It can be viewed as an effective complementary tool for those chiropractors seeking to add to their therapeutic repertoire.
Trigenics®, developed in the early 1990s, is referred to by its founder, chiropractor Dr. Allan Oolo Austin, as an interactive neurological treatment system. It can be viewed as an effective complementary tool for those chiropractors seeking to add to their therapeutic repertoire.
Aiming to correct aberrant sensorimotor and neurokinetic function, Trigenics works as a stand-alone therapy for common pain syndromes and ailments involving the neuromuscular system, and it also can serve to facilitate and sustain the adjustment. These benefits are realized through a synergistic blend of the theoretical and practical applications of functional reflex neurology, breathing biofeedback, and mechanoreceptor manipulation. Unique among manual muscle therapies, Trigenics focuses on aberrant neurology linked to dysfunctional muscle mechanoreceptors reflected in the dysefferent neuromuscular response.(1) Altering afferent input at the muscle spindle level causes normalization of neuronal tone and the improvement of any symptoms that are a result of dysfunction within this afferent-efferent neurological feedback loop. Dysafferentation has been defined as an imbalance between nociceptive information and mechanoreceptor stimulation at a spinal level.(2) In this light, benefits resulting from the chiropractic adjustment would stem from the influence of spinal articular manipulation on mechanoreceptor activity within the joints, or within the intrinsic spinal musculature.(3) The proponents of Trigenics suggest that there is also a need to normalize afferent transmission and neurokinetic function in the larger stabilizers and movers of the spine. The Trigenics practitioner applies the principles of both mind-based and body-based therapies to affect the peripheral and central nervous systems simultaneously. At a peripheral level, spinal reflex mechanisms are recruited to “quiet” the specific neuromuscular segment that is being addressed. At the same time, the patient is encouraged to perform creative visualization and practise basic biofeedback breathing techniques. By synergistically combining these components, the effect is to achieve relaxation in the entire nervous system, thereby re-establishing the function of the afferent-efferent neural reflex system. The patient typically experiences an immediate reduction in pain and discomfort, and an increase in range of motion (ROM) and strength.
Optimization of the resting and dynamic length-tension relationships of the sensorimotor system not only enhances neural afferentation but also incites proper biomechanical function throughout the body’s entire neurokinetic chain. “A variety of reflex-related structures (receptors) are contained in the muscle to sense length (muscle spindles) and tension (Golgi tendon organs),” writes University of Waterloo researcher Dr. Stuart McGill. “These modulate the stretch reflex, and when integrated with the proprioceptive system, form complex responses that facilitate or inhibit different muscles.”(4) An abnormal length-tension relationship in a muscle, produced by aberrant afferent-efferent neurological activity, can be the direct result of abnormal receptor function. This, in turn, may create an inherent “weakness” (inhibition) or “shortening” (facilitation) in the motor unit, such that the efficiency, power, and responsiveness of the muscle are negatively affected – subluxation may then result at the involved joint. Furthermore, if the muscles that are identified as weak or short are important components of the postural loading system of the axial skeleton, patterns of tightness or imbalance may lead to any number of the postural “cross-syndromes” suggested by Vladimir Janda.(5) When Trigenics is used to address these areas for postural correction, some patients actually say they feel taller post-treatment.
ASSESSMENT PROTOCOL
In addition to the usual history taking, postural observation, muscle and joint palpation and orthopedic testing, during the initial visit, a Trigenics patient is challenged with eccentric muscle-loading tests. A muscle is deemed to be inhibited or “weak” if it does not immediately respond reflexively to an eccentric load that ranges from light to moderate. Facilitated or “shortened” muscles are detected with ROM testing. Once areas of weakness and shortness are identified and charted, this bodymap of neurokinetic imbalance is used by the Trigenics practitioner to balance the body with appropriate lengthening or strengthening procedures. The muscles are retested after each application and at the beginning of subsequent treatments. The treatment plan is deemed a success when neurokinetic imbalances are no longer present, as indicated by the same muscle testing protocols. Typically, for the patient, this corresponds with a significant reduction of presenting symptoms, a correction of postural imbalances, and an overall sense of well-being. The course of treatment will depend upon the nature of the condition, and the patient’s compliance with remedial stabilization exercises and stretches.
Trigenics is relatively easy to learn, is easy on both practitioner and patient, and enhances the healing effects of the overall treatment plan that is already underway. It also opens up possibilities for treating conditions that are not normally amenable to the chiropractic adjustment.
References:
1. Austin A. Trigenics Theory Manual, Trigenics Institute of Myoneural Medicine, Toronto, 2005.
2. Seaman D. Joint complex dysfunction, a novel term to replace subluxation/subluxation complex: Etiological and treatment considerations. J Manipulative Physiol Ther 1997; 20:634-44.
3. Seaman DR, Winterstein JF. Dysafferentation: A novel term to describe the neuropathophysiological effects of joint complex dysfunction. J Manipulative Physiol Ther 1998; 21(4):267-280.
4. McGill S. Ultimate Back Fitness and Performance, Backfitpro Inc., 2006.
5. Morris CE, Greenman PE, Bullock, MI, Basmajian JV, Kobesova, A, Janda V. Tribute to a master of rehabilitation: historical perspective. Spine 2006; 31(9):1060-1064.
Print this page