
How to assess and treat marathoners
By Anthony J. Lombardi & Richard Lebert RMT
Features Clinical Techniques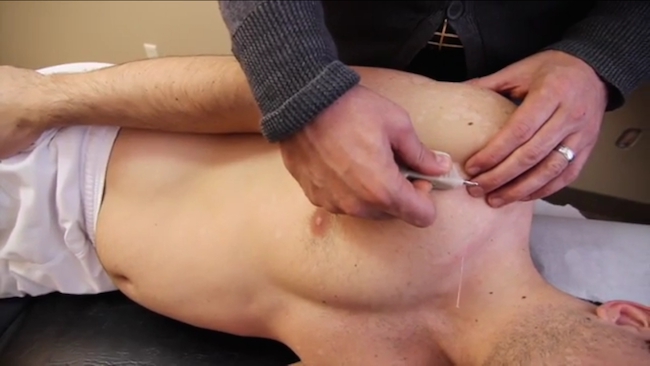
Many chiropractors treat recreational or amateur athletes. Often, they encounter patients that have injuries that stem from overuse or improper movement mechanics.
This is very apparent in marathon and long distance runners. For instance, the average serious marathon athlete takes 16 weeks to prepare for a race and averages about 50 kilometers per week. During the many months of preparation they are seemingly able to power through any training-related injuries, pain and dysfunction. But once the race is done, they take a rest – that’s when everything falls apart mechanically.
In the March 2013 issue of the Journal of the American Chiropractic Association, I (Lombardi) wrote a paper titled, “Adapted Musculoskeletal Systems: Causes and Restoration.” The article recommends that chiropractors and therapists take an updated approach to how they assess and treat musculoskeletal injuries when athletes are experiencing pain and dysfunction.
The heat is on
It’s been inferred there is a physiological reason why long distance runners “fall apart” after weeks of training their musculoskeletal systems. The analogy of a steel mill is often used to describe this phenomenon. In a steel mill there is a blast furnace that runs at temperatures above 800 degrees Celsius to cook the impurities from the steel during manufacturing. These blast furnaces are primarily made of bricks and mortar and the furnace never completely shuts off, because once it stops running the furnace would simply fall apart from the damage of the heat and the overuse over time.
In a blast furnace, it’s the heat and the continuous use that keeps the furnace together and allows it to run. The same is true for endurance athletes and marathoners. Athletes who overtrain often have problems in the two weeks following the competition because while they are in training, physiologically, the body is releasing adrenalin, endorphins and neurotransmitters – which prime the nervous system to ensure that the muscular system remains functional. In addition, athletes usually practise good nutrition and their continuous training stimulates the production of collateral blood vessels through angiogenesis. So, they are able to feed their tissues, allowing them to perform well on a daily basis.
Function junction
This is why it is clinically important to assess these athletes functionally – but it’s also paramount to assess them globally. For instance, Carvalhais et al recently demonstrated a term called strain transmission in which muscles from opposite areas of the body affect one another’s individual function.
Something we routinely find in practice are long distance runners whose chief complaint is gluteus maximus pain, which is associated with an inhibited serratus anterior muscle on the same or opposite side. Over a training period, the average runner will take 600,000 strides over 16 weeks. Research from Hurley, Nijs and others demonstrate how repeated movements and pain can cause muscular motor inhibitions at neuromuscular junctions. Thus, repeated movements, such as 600,000 strides, can contribute to and magnify musculoskeletal mal-adaptations in the upper and lower extremities.
Motor inhibition
Motor muscle inhibition (alpha-motor neuron muscle inhibition) happens when the nerve that sends the impulse to contract the muscle becomes unable to function at its optimal capacity due to chemical or physical trauma. Direct or repetitive trauma or changes in the joint, like inflammation, swelling or arthritis, will decrease motor output. Therefore, any trauma, pain, nociception or neurogenic inflammation in the region of the joint or muscle belly can trigger a modification of afferent information within the muscle spindles – causing motor inhibition.
How to assess and fix
A small mechanical dysfunction may alter the viscosity of the loose connective tissue within fascia. Pavan and Nijs feel that this may be a potential source of nociception due to the stimulation of embedded nerve receptors that can mesh within pathological changes. This ongoing peripheral pathology has the potential to affect motor output. Many chiropractors and massage therapists are now using a functional assessment approach, which considers the dynamic interaction of structure and function and how this relationship influences the athlete’s adaptive capacity. Functional assessment is a reliable and reproducible way to assess for changes in motor output before they can magnify into a gigantic problem down the road.
Runners are a meticulous group that notice when something is starting to “feel off” – even if they cannot pin-point the local dysfunction. For instance, functional assessment is used to locate dysfunction by testing active muscle recruitment patterns. Then the treatment target is selected by palpating for a local induration of the soft tissue and focusing on inhibited motor points (neuromuscular junctions). However, because running requires the entire body it is extremely advisable to assess motor function in upper and lower extremities – especially at the shoulder and pelvic girdles.
Oak Point Method
Dimitri Boules, a massage therapist and acupuncturist from New York City has just published his book called The Oak Point Method. In the book he has a chapter dedicated to the Exstore System and uses it to treat many of the runners in the New York City Marathon.
In the Oak Point Method, Boules describes how using motor point acupuncture brings instant results to the patients subjective and objective findings because it restores sensory-motor integration at the neuromuscular junction.
“As far as my personal experience with marathon runners, I most commonly see athletes with IT band pain but 100 per cent of them always have weakness on the ipsilateral TFL, gluteus medius and gluteus minimus muscles. I attribute that to the repeated sagital movements during their training. After I restore the areas of dysfunction using electro-acupuncture – I do a local treatment on to the lateral knee. The local treatment is a combination of acupuncture and some kind of manual therapy.”
If you have any questions for Dimitri Boules he can be contacted on Instagram @oakpointhealth and Richard Lebert can be reached @adaptivetherapy. Dr. Lombardi can be emailed – exstore@usa.com
Dr. Anthony Lombardi has presided over 98,000 patient visits in 13 years of practice at Hamilton Back Clinic.
Print this page